The Importance of Hormonal Balance in Women’s Health
Hormones are very important for every aspect of women’s health as they influence fertility, mood, metabolism, bone density, and heart health. Although hormonal fluctuations are natural, excessive disruption of normal hormonal cycles can precipitate a range of health concerns.
According to research published in peer-reviewed journals such as Frontiers in Medicine and data from large-scale studies, hormonal balance is critical to a woman’s physical and emotional well-being.
In this article, we will explore how hormonal balance impacts women’s health, common conditions that arise from hormone imbalances, and what women can do to take proactive roles in the management of their endocrine health.
Understanding Hormonal Regulation
A healthy menstrual cycle depends on precisely timed connections between the hormones that are secreted by the hypothalamus, pituitary gland, and ovaries. In adolescence, the hypothalamic-pituitary-ovarian axis gradually matures, which establishes regular ovulatory cycles by around age 18.
As estrogen and progesterone rise and fall, they orchestrate endometrial thickening and shedding. These two processes are vital for reproductive health. Conversely, disturbances in this cycle (due to stress, lifestyle, endocrine disorders, and exogenous hormones) can impair fertility and signal deeper health concerns.
What Hormones Impact Women’s Health
Estrogen: Supports reproduction, bone density, and cardiovascular function [R].
Progesterone: Counters estrogen’s proliferative effects on the uterus and stabilizes cycles.
Testosterone (in lower amounts): Contributes to libido, muscle integrity, and mood regulation.
Thyroid Hormones: Control metabolic rate and energy levels.
Cortisol: The “stress hormone” regulates immune response and metabolism.
Check out information about stress and cortisol by clicking on this link (insert link).
Potential Disruptors to Hormonal Balance
Although hormonal levels can be affected by factors such as poor diet, chronic stress, and lack of sleep, a major disruptive element is hormonal therapy (combined estrogen-progestin contraceptives and progestin-only formulations).
By design, these contraceptives create an artificial state of anovulation. Studies indicate they may accelerate ovarian aging markers and trigger various side effects:
Ovarian Reserve Changes
Long-term use of combined oral contraceptives can reduce serum antimullerian hormone (AMH) and modify cervical mucus. This makes it harder for some women to conceive quickly after discontinuation.
Metabolic Shifts
Synthetic estrogen and progestins may increase insulin resistance in susceptible individuals, which contributes to weight gain and metabolic complications.
Elevated Cardiovascular and Oncological Risks
Some formulations appear to raise the risk of venous thrombosis, hypertension, and certain hormone-sensitive tumors (e.g., breast and cervical cancers).
Hormonal Balance Across a Woman’s Life
Adolescence
Hormonal fluctuations at menarche (the first menstrual cycle) can cause irregular periods, mood swings, and acne. As the body matures, hormones generally stabilize.
Reproductive Years
Regular ovulation cycles usually indicate healthy hormonal rhythms. Contraceptive medications or certain medical conditions such as Polycystic Ovary Syndrome (PCOS) and endometriosis may alter hormone levels.
Pregnancy and Postpartum
Dramatic shifts in estrogen, progesterone, and other hormones occur to support fetal development and breastfeeding. Postpartum hormone drops can sometimes trigger mood swings or postpartum depression.
Perimenopause and Menopause
Estrogen and progesterone decline, which commonly causes symptoms such as hot flashes, mood changes, and sleep disturbances.
Common Hormone-Related Conditions in Women
Women can experience various endocrine disorders. Some examples include:
PCOS
This condition is characterized by high androgen levels and insulin resistance. The hallmark symptoms manifest as irregular periods, acne, weight gain, and fertility issues.
Learn more about PCOS by clicking here.
Endometriosis
Although this condition is not always described as a hormone imbalance, estrogen dominance and inflammatory factors can play a role in abnormal tissue growth outside the uterus.
Thyroid Disorders
Hypothyroidism and hyperthyroidism can occur at any age. However, the risk may rise with advancing age or a family history of thyroid problems.
Osteoporosis
Lower levels of estrogen after menopause accelerate bone density loss, which increases the risk of fractures.
The accurate identification of these disorders requires:
Blood tests for thyroid function (T3/T4).
Check LH/FSH for ovarian function.
Evaluate insulin and fasting glucose in suspected PCOS.
Imaging tests to observe abnormal growth/shrinkage of endocrine glands.
What Affects Hormonal Balance in Women?
Stress
Chronic stress directly leads to elevated cortisol, which can disrupt the delicate interplay of estrogen and progesterone.
Body Weight and Composition
Fat cells (i.e., adipose tissue) can produce extra estrogen. If you are underweight, it can also cause low estrogen levels, which could sometimes halt menstruation (i.e., amenorrhea).
Diet and Nutritional Intake
Adequate protein, omega-3 fatty acids, fiber, and certain vitamins (e.g., vitamin D) help stabilize hormones. Excess sugar and refined carbs can provoke insulin spikes, which contribute to imbalances.
Physical Activity
Sedentary lifestyles and overtraining can disrupt hormone levels, which affects menstrual health, bone density, and mood.
Contraceptive Use
Hormone-based contraception, such as combined oral contraceptives or hormonal intrauterine devices, can:
Suppress ovulation.
Lead to changes in cervical mucus.
Alter insulin sensitivity and mood.
Although many women safely use hormonal contraceptives, certain adverse effects (e.g., depression, shifts in libido) may occur.
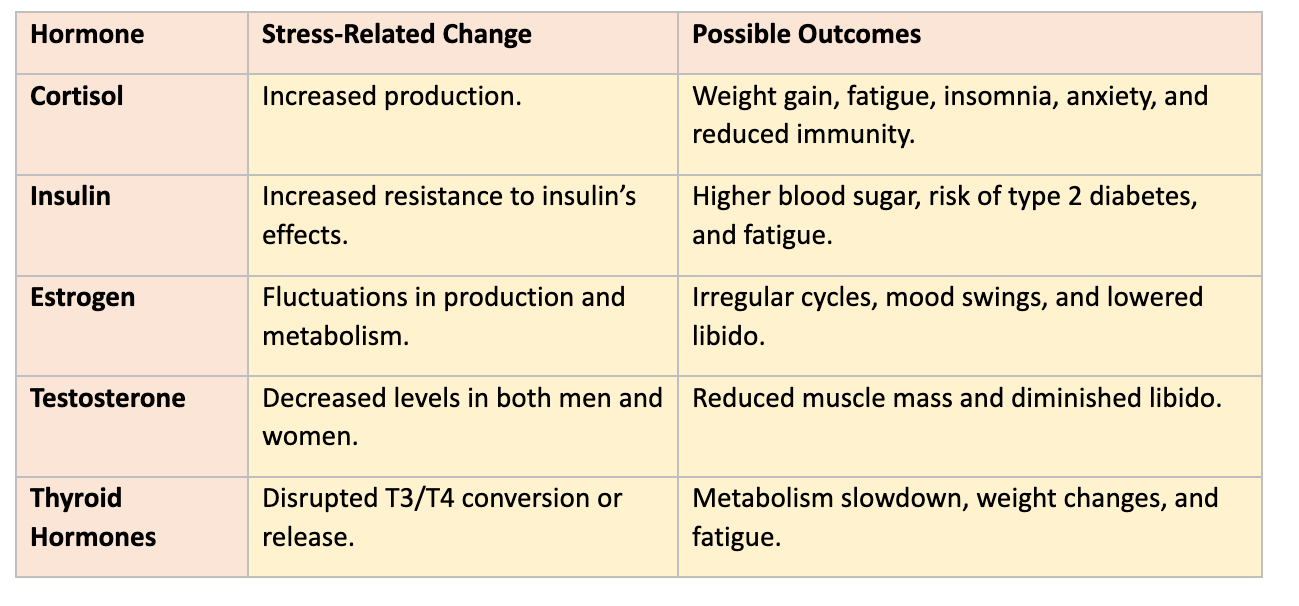
Here are the potential effects of hormonal imbalance in women:
Takeaway Message
Hormonal balance is a foundation of women’s health that influences everything from adolescence to menopause. When we understand how hormones function, women are better equipped to act as advocates for their own well-being.
Lifestyle interventions such as healthy eating, regular physical activity, and effective stress management are powerful first-line tools to preserve hormonal balance. Moreover, routine screenings, thorough patient education, and supportive healthcare relationships ensure early detection of potential issues.
Ultimately, each woman’s endocrine journey is unique, which is why it’s critical to follow a personalized approach.
If you have any questions about how hormonal balance impacts women’s health, please feel free to share your thoughts in the comment section below or reach out to us via this link.
Caring for Your Endocrine Health – A Beginner’s Guide
The endocrine system is a complex network of glands that produce, store, and release hormones. These chemical messengers regulate numerous processes, including:
Growth.
Metabolism.
Reproduction.
Mood.
Stress response.
Because hormones directly impact so many physiological and psychological functions, it is indispensable to take care of your endocrine health. Unfortunately, many people are unaware of how hormonal imbalances may present themselves and what steps they can take to maintain healthy endocrine function.
In this article, we’ll discuss the basics of the endocrine system, common endocrine disorders, and simple lifestyle measures that can help you maintain hormonal balance. We will also touch on the importance of patient autonomy and the right to accurate and evidence-based information about endocrine health.
Understanding the Endocrine System
The endocrine system is composed of multiple glands, including:
Pituitary gland – This is referred to as the “master gland.” The pituitary gland secretes hormones that influence growth, reproductive functions, and stress responses.
Thyroid gland – Regulates metabolism, energy levels, and protein synthesis.
Adrenal glands – Produce cortisol (i.e., the stress hormone) and aldosterone (an important hormone for blood pressure and electrolyte balance).
Pancreas – The pancreas has both endocrine and exocrine functions. The most important role is to regulate blood glucose.
Ovaries and Testes – These glands are involved in reproductive hormone production such as estrogen, progesterone, and testosterone.
Pineal gland – Releases melatonin, which helps regulate sleep cycles.
Each of these glands secretes hormones into the bloodstream, which allows them to travel throughout the body and activate target cells. When hormone levels fall out of their normal ranges due to overproduction or underproduction, symptoms of endocrine disorders can arise.
Signs and Symptoms of Endocrine Imbalance
Hormonal imbalances can be subtle or severe. Some common signs and symptoms include:
Unexplained weight changes (loss or gain).
Chronic fatigue or insomnia.
Changes in mood (e.g., anxiety, irritability, depression).
Irregular menstrual cycles and low libido.
Distractibility (i.e., feeling “foggy”).
Dry skin, hair loss, and brittle nails.
High blood pressure and irregular heart rate.
Although these symptoms can have many causes, persistent symptoms could be a sign of an underlying endocrine issue and should be evaluated by a healthcare professional.
The following table summarizes some frequently encountered endocrine disorders, associated hormones, and main symptoms:
Keep in mind that each of these conditions requires a thorough medical evaluation and specialized treatment. Your primary care physician or endocrinologist are best fit to manage these conditions.
How to Maintain a Healthy Endocrine System
Balanced Nutrition
A diet that’s rich in whole grains, lean proteins, fruits, and vegetables supports hormonal balance. Some micronutrients (e.g., iodine for thyroid function, calcium and vitamin D for bone health) are absolutely vital.
Excess sugar and refined carbohydrates can stimulate insulin surges and affect blood glucose regulation, so moderation is very important.
Regular Physical Activity
Exercise regulates insulin sensitivity, maintains a healthy weight, and reduces stress. Walking, swimming, and resistance training can all be beneficial on various hormone levels, including cortisol and insulin.
Stress Management
Chronic stress raises cortisol levels, which can disrupt other hormonal pathways. Mindfulness techniques such as meditation, deep breathing exercises, and yoga can help mitigate chronic stress and maintain balanced cortisol levels.
Adequate Sleep
Sleep is extremely important for hormone regulation, especially growth hormone, melatonin, and cortisol. Make sure you get 7–8 hours of quality sleep per night. Also, try to maintain a consistent schedule.
Learn more about the connection between sleep and hormones by clicking here (insert a link).
Limit Environmental Toxins
Chemicals in personal care products, plastics, and pesticides (i.e., endocrine disruptors) may mimic or interfere with hormone activity. Therefore, we recommend that you lower your exposure to these chemicals. You can do that by choosing products that are labeled as “BPA-free.” You could also buy organic produce when it’s possible.
Regular Checkups
If you have a family history or symptoms that suggest any endocrine disorders, regular screening and lab work can help detect issues early. It is critical to work closely with your endocrinologist to monitor changes over time.
Patient Autonomy and Communication
When it comes to endocrine health, every individual has the right to understand their treatment options, possible side effects of medications, and lifestyle changes that might benefit them.
Open communication with healthcare providers ensures that patients can make informed decisions. As some research indicates, there is a need for healthcare professionals to provide comprehensive information about the potential side effects of hormonal treatments (e.g., oral contraceptives, thyroid medication).
Healthcare professionals and patients should work together to promote trust and ensure better health outcomes. If you have questions about your hormone levels or any prescribed therapy, do not hesitate to speak up. You can request second opinions, discuss alternative treatments, or simply share any side effects you may be experiencing.
Takeaway Message
Caring for your endocrine system is not a luxury. Think of it as fundamental to your health. Since hormones influence nearly every function (e.g., digestion, metabolism, mood, reproduction), a focus on balanced nutrition, regular exercise, stress management, and open communication with healthcare professionals can go a long way to support hormonal balance. Make sure to learn about the common endocrine disorders, their warning signs, and how to advocate for your own health.
We hope that this article managed to shed some light on the most common endocrine conditions and how to manage them appropriately.
If you have any questions or concerns about any endocrine symptoms, please feel free to share your thoughts by reaching out to us.
How Stress Affects Your Hormones and What You Can Do About It
Stress is an inescapable part of modern life. Today, we have to deal with daily work deadlines, family responsibilities, and unexpected life events. However, what many don’t realize is that stress can directly affect our hormonal balance. When stress becomes chronic, it can contribute to hormonal imbalances that negatively impact mood, energy, metabolism, and even reproductive health.
In this article, we explore the physiological mechanisms that make stress very disruptive to hormonal balance as well as the signs and symptoms of stress-induced hormonal imbalances.
The Biology of Physical and Psychological Stress
When you encounter a stressful situation (physical, emotional, or psychological), your body initiates the so-called “fight-or-flight” response. This involves a rapid increase in cortisol and adrenaline, which are mainly released by the adrenal glands.
As a short-term response, these hormones:
Raise your heart rate.
Increase alertness.
Redirect blood flow to essential muscles.
However, in chronic stress situations, this constant surge in cortisol triggers a cascade of hormonal changes that affect multiple processes:
Thyroid Function: Excess cortisol can disrupt thyroid hormones and lower metabolic rate.
Insulin Sensitivity: Chronically high cortisol may precipitate insulin resistance, which causes weight gain and elevated blood sugar.
Sex Hormones: Hormones such as estrogen and testosterone can become imbalanced. As a result, you may experience reduced libido and reproductive issues.
Mental Health: Abnormally high cortisol over long periods is associated with higher risks of depression, anxiety, and even suicidal ideation.
Consequences of Chronic Stress on Hormones
Stress affects other hormones aside from cortisol. It can set off a domino effect that involves nearly all major hormonal axes. As a result, it disrupts the delicate balance within the endocrine system.
Here is a detailed discussion of stress’ impacts on different hormones:
Disrupted Menstrual Cycle or Low Libido
When your body faces chronic stress, reproductive functions can be diminished as the body reallocates resources toward the management of stressors rather than reproduction.
Adrenal Fatigue
Though the term “adrenal fatigue” is still debated, some people do experience adrenal insufficiency or dysfunction. These conditions are characterized by persistent fatigue and difficulty managing stress.
Learn everything there is to know about adrenal fatigue by clicking on this link.
Weight Fluctuations
Chronically elevated cortisol increases cravings for high-calorie foods, which promotes weight gain or difficulty losing weight.
Insomnia and Poor Sleep Quality
Elevated stress hormone levels can disrupt your natural sleep-wake cycle. Consequently, you may struggle with insomnia or non-restorative sleep.
This table summarizes the common hormonal changes that may occur due to chronic stress:
Stress-Induced Hormonal Imbalances
It’s vital to identify when stress is at the root of your hormonal issues. Some clues include:
High anxiety or depressed mood without a clear cause.
Changes in menstrual cycles (e.g., onset of perimenopausal symptoms that seem premature).
Inability to focus or experience memory lapses (may be referred to as brain fog).
Poor exercise tolerance despite high fitness levels.
Unexplained changes in appetite (either significant increase or decrease).
If you suspect chronic stress is responsible for the disruption of your endocrine health, consider a consultation with an endocrinologist. Blood tests measure cortisol, thyroid function, and reproductive hormone levels, which are very effective in the diagnosis of hormonal imbalances.
How to Combat Stress-Driven Hormone Imbalances
Lifestyle Modifications
Prioritize sleep and make sure that you get 7–8 hours of uninterrupted rest. Poor sleep can heighten cortisol levels.
Manage your time and develop realistic schedules to prevent feelings of overwhelm.
Incorporate whole foods that support stable blood sugar, such as vegetables, lean proteins, and complex carbohydrates.
Mind-Body Techniques
Meditation and mindfulness-based practices help lower perceived stress and cortisol.
Yoga or Tai Chi are considered gentle forms of exercise that encourage relaxation and improve mental clarity.
Regular Exercise
Moderate-intensity exercises such as walking, jogging, and swimming help regulate cortisol over the long term.
Avoid excessive or high-intensity workouts, which may exacerbate stress in susceptible individuals.
Social and Emotional Support
Counseling and therapy could help you manage chronic stress and build coping strategies.
Community and group activities could help you become more resilient to life stressors.
Medical Interventions
If lab tests confirm severe imbalances (e.g., adrenal insufficiency or thyroid disease), a doctor may prescribe pharmacological drugs.
Stress management programs provide structured stress management or biofeedback programs.
Do Not Fall for Information Overload
Today, patients frequently encounter conflicting advice. Although online resources can be helpful for background research, they also risk the oversimplification or sensationalization of data. Therefore, it is absolutely vital that you consult with a reputable healthcare professional to make sure that you are getting the best-personalized advice based on an evidence-based approach.
It’s also important to maintain autonomy over your health choices. If a prescribed medication or supplement doesn’t feel right, ask questions, request a second opinion, and explore alternative evidence-based therapies. However, you must not stop your medications without first consulting with your doctor.
Takeaway Message
Stress can have deep ramifications on hormone levels, which could affect many aspects of your health, including mood, weight, and reproductive health. When you become aware of the interplay between stress and hormones, you can recognize early warning signs and take proactive measures. The adoption of a balanced lifestyle that covers proper sleep, nutritious foods, regular exercise, and effective stress management tools serves as your foundation for healthy hormone function.
If you have any questions or concerns about the effects of stress on your health and well-being, we recommend that you reach out to your endocrinologist for personalized advice. You can also reach out to us via this link for a private conversation.
How to Manage Diabetes – Tips from an Endocrinologist
The management of diabetes requires a comprehensive approach that goes beyond dietary changes. As you monitor your carbohydrate intake, you should also focus on foods with a low glycemic index (GI). Additionally, regular physical activity, adequate sleep, and stress management techniques can all support glycemic control. Working closely with an endocrinologist is vital to address the many variables that affect blood glucose.
In this article, we’ll briefly break down the concept of the glycemic index, explore the benefits of a low-GI diet, and discuss other beneficial ways to manage diabetes, according to an endocrinologist.
The benefits of a low glycemic index diet
As endocrinologists, we always recommend that our diabetic patients follow a low glycemic index diet.
However, individuals who are already taking insulin and significantly change their eating patterns
without adjusting their insulin dosages may be at an increased risk of low blood sugar.
Additionally, if cholesterol levels rise after you adopt a low-carbohydrate diet (e.g., the keto diet), it
might not be a suitable choice for you.
Foods with a low glycemic index
Milk
Skimmed milk has a GI score of 37, whereas full-fat milk scores 39. Milk is an excellent source of calcium, which plays a vital role in bone health. Researchers found that regular milk consumption may slow the development of osteoarthritis in women.
Chickpeas
Chickpeas (i.e., garbanzo beans) are a low-GI legume with a score of 28 on the glycemic index. Not only do chickpeas have a low GI score, but they are also rich in protein and fiber, providing 11.8 grams and 10.6 grams per cup, respectively. They contain essential nutrients, including calcium, potassium, and folic acid. Chickpeas can be used as a substitute for high-GI foods, such as potatoes or white rice. Roasted chickpeas make for a quick and easy snack. Another delicious way to incorporate chickpeas into your diet is by making hummus. This popular Middle Eastern dip is easy to prepare.
Kidney beans
Kidney beans have a GI score of 24. These beans are high in protein, with up to 13.36 grams per cup, and contain 11 grams of fiber. They are also rich in potassium and low in fat. Kidney beans are an excellent choice for both meat-based and vegetarian chilli.
Lentils
Lentils are a great food to incorporate into your lunch and dinner, with a GI score of 32. Lentils are rich in protein, providing 17.86 grams per cup. They make up a great source of fiber, offering 15.6 grams per cup. They also contain phosphorus and potassium. One way to enjoy lentils is through an Indian dish called dhal.
Stay Active
Aim for at least 30 minutes of moderate exercise most days of the week. Examples include brisk walking, cycling, swimming, and low-impact aerobics. If you’re new to exercise or have physical limitations, begin with 10-minute sessions of gentle walking and gradually increase your time and intensity. Consider a fitness tracker or a simple pedometer to count steps and stay motivated. You can also Incorporate strength training (e.g., light resistance bands, bodyweight exercises) twice a week to build lean muscle, which can further improve insulin sensitivity. If you spend much of your day seated, try standing or stretching breaks every hour.
Prioritize Sleep
Adults need 7–9 hours of quality sleep per night. Stick to a consistent bedtime and wake-up schedule (even on weekends) to regulate your body’s internal clock.
How to Improve Sleep Quality
Create a calming bedtime routine. Lower the lights, read a book, and listen to soothing music. Avoid heavy meals, caffeine, and intense exercise within a few hours of bedtime. Keep electronics out of the bedroom or switch them off 30 minutes before bed.
Ensure your room is dark, quiet, and cool (around 65°F/18°C is recommended). If you struggle with insomnia or suspect sleep apnea, consult a healthcare professional for targeted solutions.
Sleep impacts hormones that control hunger (ghrelin and leptin) and stress (cortisol). Poor or inadequate sleep can disrupt these hormones, which precipitates higher blood sugar and increased appetite.
Manage Stress
Incorporate stress-reduction techniques such as deep breathing, yoga, meditation, and progressive muscle relaxation into your daily routine. Even five minutes a day can make a difference.
Start simple. For deep breathing, sit comfortably, inhale slowly for a count of four, hold for a count of two, and exhale for a count of four. Repeat for several cycles. If you prefer guided sessions, explore mobile apps or online videos that teach mindfulness and relaxation techniques.
Monitor Your Blood Sugar
Check blood glucose levels as advised by your healthcare provider, which may be multiple times a day if you use insulin or once a day/once every few days for diet-controlled diabetes.
Use a glucometer or continuous glucose monitor (CGM). Keep a record of readings to track patterns, especially before and after meals, exercise, and stressful events.
To further improve your diabetes management, bring your glucose log to medical appointments. Discuss any unusual trends (e.g., consistent morning highs or post-meal spikes) with your doctor or endocrinologist for targeted advice.
Adhere to Medication and Checkups
Take oral medications or insulin exactly as prescribed. Do not skip doses. Also, never adjust dosages on your own without a consultation with a healthcare professional.
Set phone alarms or use a pill organizer to manage multiple medications. Keep an updated medication list and share it during medical appointments to avoid drug interactions or errors.
Visit your endocrinologist or primary care physician for HbA1c tests, blood pressure monitoring, cholesterol checks, and other routine assessments. Early detection of complications (e.g., nerve damage, eye problems) is indispensable to prevent complications.
Here is a table that summarizes all the tips that we covered above:
Takeaway message
The management of diabetes requires that you follow the tips of professional healthcare providers, which include low-GI meal planning, regular exercise, sufficient sleep, stress management, and consistent blood sugar monitoring.
We hope that this article successfully highlighted the best tips to manage diabetes from a board- certified endocrinologist.
Top 5 Myths About Diabetes – You Need to Stop Believing
Diabetes is a chronic condition where the body cannot produce enough insulin or use it properly. This causes chronically elevated blood sugar levels.
Nearly 5,000 Americans are diagnosed every day with diabetes. Staggeringly, more than 11.6% of the U.S. population lives with type 1 or type 2 diabetes. That’s more than 38 million people. Despite its prevalence, various myths are spread all over the internet.
In this article, we will cover the five most common myths that surround diabetes. After that, we will fact-check each myth and share some helpful tips to manage your blood sugar levels.
1. Myth: “Eating Too Much Sugar Directly Causes Diabetes”
Reality
Although excessive sugar can lead to weight gain, which is a major risk factor for type 2 diabetes, sugar alone isn’t the singular cause. Other factors such as genetics, age, and physical inactivity are direct contributors. What’s more, type 1 diabetes is autoimmune, which means it has nothing to do with sugar intake.
What You Need to Do
A balanced diet and regular exercise matter more than obsessively avoiding sweets. Occasional indulgences won’t automatically cause diabetes. However, if you consistently exceed your calorie needs, the risk of type 2 diabetes will definitely increase.
2. Myth: “Only Overweight People Get Diabetes”
Reality
Overweight individuals are at a higher risk of type 2 diabetes. However, many people at a healthy weight can also be diagnosed. Genetic predisposition and lifestyle factors such as inactivity can override body size. Conversely, some obese individuals never develop diabetes. According to the Centers for Disease Control and Prevention (CDC), up to one-third of obese individuals never develop type 2 diabetes.
What You Need to Do
Weight is only one piece of the puzzle. Active living, balanced meals, and regular checkups can help you maintain optimal blood sugar levels regardless of your body type.
3. Myth: “Once You’re Diabetic, You Can’t Reverse It”
Reality
Type 1 diabetes requires lifelong insulin. This is because the immune system will produce cells that attack the islets of the pancreas that produce insulin (i.e., beta cells). Therefore, there is little to no insulin in your bloodstream to regulate glucose levels. That means that the only way to lower your glucose after a meal is by artificially injecting it. However, many with type 2 diabetes can achieve remission, especially if they address risk factors early. Prediabetes describes a borderline state of elevated glucose. This condition can be reversed through healthier diets and consistent physical activity.
What You Need to Do
Not all forms of diabetes are permanent in the same way. Even if remission occurs, ongoing monitoring is indispensable as high blood sugar can return if habits slip.
4. Myth: “People with Diabetes Must Eat Special ‘Diabetic-Friendly’ Foods”
Reality
Specialized “diabetic” products are expensive and not necessarily healthier. A balanced diet of vegetables, fruits, whole grains, lean protein, and healthy fats benefits everyone, including those with diabetes. Foods that are labeled “sugar-free” may contain sugar alcohols or unhealthy fats.
What You Need to Do
It’s more effective to watch portion sizes and ingredients than to rely on “diabetic” labels. A nutrient-rich menu is a better strategy for stable blood sugar.
5. Myth: “Exercise Isn’t Safe if You Have Diabetes”
Reality
On the contrary, physical activity significantly improves insulin sensitivity, helps with weight control, and supports heart health. Those who use insulin or certain medications can prevent low blood sugar through glucose monitoring and dose adjustments. Low-impact exercise such as walking or swimming is actually ideal for those who are concerned about joint or nerve issues.
What You Need to Do
Exercise is vital to good diabetes management. The benefits include improved blood sugar control and cardiovascular health, which far outweigh the potential downsides.
Practical Tips to Manage Your Blood Sugar Levels
Monitor Blood Sugar
Use a home glucose meter for daily checks and get HbA1c tests as recommended. Tracking trends helps personalize your care.
Balance Your Meals
Emphasize fiber-rich foods like vegetables, fruits, and whole grains. Limit refined carbs and saturated fats.
Stay Hydrated
Water is best. Sugary drinks can spike glucose and provide excess calories.
Focus on Heart Health
Diabetes raises the risk of cardiovascular disease. Therefore, we recommend that you adopt heart-friendly eating and keep your blood pressure in check.
Address Mental Wellness
Stress can impact blood sugar. Techniques such as meditation, counseling, and group support can help keep you on track.
Consult Professionals
Work closely with doctors, dietitians, and diabetes educators for personalized advice. Medications or insulin adjustments may be necessary.
Conclusion
Myths about diabetes can create unnecessary fears or precipitate harmful choices. In reality, diabetes occurs because of many factors, including genetics, weight, and lifestyle. Although sugar intake should be monitored, it’s not the sole contributor. Excessive calories from any source can be problematic.
We hope that this article will serve as a guideline to debunk the most common myths about diabetes as well as a few practical tips to better manage your blood sugar levels.
If you have any questions or concerns about type 1 or type 2 diabetes, feel free to reach out to us via this link.
The Link Between Hormones and Sleep – How toImprove Your Rest
Suffering from insomnia is a real public health crisis. The frustrating feeling of wanting to sleep but not being able to can be quite daunting. Unfortunately, it can be difficult to pinpoint what’s wrong. For this reason, you need to understand the role of cortisol and melatonin in this ordeal. Irritability when you are asleep and feeling tired but wired could be the result of hormonal imbalance. To put it simply, high levels of cortisol or low levels of melatonin during the evening. The opposite also produces similar effects. In this article, we will cover some of the methods that allow you to balance your hormones, especially cortisol and melatonin.
How Stress Affects Cortisol and Sleep
When you are under constant stress (whether from work, personal issues, or health challenges), your body releases higher amounts of cortisol. This hormone is meant to help you cope with immediate threats. However, chronic elevation can disrupt your circadian rhythm. Over time, elevated evening cortisol levels make it harder to unwind, which creates that “tired but wired” feeling. Consequently, you may have difficulty initiating sleep or experience frequent awakenings throughout the night.
The balance of cortisol-melatonin – How to ensure better sleep and sustained energy
Sunrise alarm clocks
Light is the main factor that determines the onset and duration of your sleep. Therefore, you can use this knowledge to trick your brain. Start by getting a sunrise alarm clock, which gradually increases the light intensity of the room until it’s time to wake up. By doing this, you will create an artificial environment that resembles the one our ancestors lived in (i.e., the jungle). Some devices even come with color grading, which changes from red to orange to bright yellow. The purpose of this feature is to follow the order of colors seen during sunrise.
Natural exposure to light
If you don’t want to get the sunrise alarm clock, you can use natural sunlight. Leave your house as soon as you wake up to get exposed to the sunlight and regulate your circadian rhythm. Of course, this is easier said than done, as most people find it very challenging to leave their beds in the morning.
Stay away from digital devices near your bedtime
The National Sleep Foundation advises people to avoid using digital devices before bedtime. Since these devices emit ultraviolet light, they can suppress the release of melatonin, which is indispensable for quality sleep.
Don’t exercise before bedtime
Exercising very late during the day increases your blood hormones, such as cortisol, epinephrine, and norepinephrine. While there is some evidence to disprove the negative effects of late-night exercise on sleep quality, it is best to avoid it. Instead, try to schedule your workout sessions earlier in the day. Optimally, you would exercise during the early morning.
Take short naps (20-30 minutes)
This one is straightforward.
A 2-hour nap in the middle of the day can alter your circadian rhythm. This gives signals to the brain that there is no need to sleep even if it’s 4 AM. The best way to combat this effect is by taking short naps, lasting for 20 to 30 minutes. This will prevent a condition known as advanced phase disorder.
Avoid stimulants near your bedtime (e.g., caffeine, nicotine)
Make sure to not consume any stimulants before your bedtime. This includes coffee, tea, cigarettes, and energy drinks. The ingredients found in these products can interfere with the normal function of your biological clock.
Note that the action of these products may last long. In other words, drinking a cup of tea at 6 PM can mess up your bedtime at 10 PM. As a result, you may experience acute insomnia that night. If these habits are not corrected, the problem can become chronic.
Speak with your physician if you are experiencing acute or chronic insomnia.
Mindfulness and Relaxation Techniques
Engage in relaxation practices to lower cortisol levels and prime your body for restful sleep. Techniques such as progressive muscle relaxation, deep breathing exercises, and guided imagery can reduce stress hormones in the bloodstream.
Note that mindfulness meditation and gentle yoga before bed can help your body and mind transition smoothly into a more relaxed state. This can improve sleep quality and duration.
When to Seek Professional Help
If lifestyle modifications don’t fix your insomnia or chronic fatigue, you should consider seeking help from a healthcare professional. Endocrine disorders, anxiety, and other medical conditions can exacerbate cortisol imbalances.
Therefore, you may need the proper evaluation to reveal underlying causes and guide you toward targeted therapies such as specialized hormonal treatments.
Takeaway message
Controlling your hormone levels is absolutely crucial to getting high-quality sleep. Ensure to speak with your primary care physician before you make any drastic changes in your diet or exercise routine.
We hope that this article helped you understand the role of cortisol and melatonin in controlling the sleep-wake cycle.
What Is Polycystic Ovary Syndrome (PCOS) and How Can It Be Treated?
Polycystic ovary syndrome, or PCOS, is a common medical condition seen in women of childbearing age (15-44). PCOS alters the normal menstrual cycle and causes a variety of symptoms.
According to studies, more than 70% of women with PCOS have not yet been diagnosed since the symptoms may be too subtle to detect.
In this article, we will discuss the causes, symptoms, and treatment options for polycystic ovary syndrome.
The causes of PCOS
Scientists are still uncertain about the exact causes that lead to PCOS. However, they managed to pinpoint the following risk factors:
Insulin resistance
The vast majority of patients with PCOS present with insulin resistance, which is the primary driver of type II diabetes.
For this reason, patients with PCOS may greatly benefit from dietary changes and exercise to lose weight and control their blood sugar levels. Subsequently, the symptoms of PCOS start to gradually disappear.
Additionally, many PCOS patients benefit from taking metformin (a drug used for diabetic patients).
Inflammation
Obesity is the number one cause of systemic inflammation, which increases the risk of PCOS.
Family history
In a 2005 study, scientists found that patients with a family history of PCOS are more likely to develop this condition than those with no family history.
Another group of scientists published a paper in 2016, suspecting several genes that lead to PCOS.
What are the types of PCOS?
Insulin resistant PCOS
Insulin-resistant PCOS is the most common type. It affects approximately 70% of patients with PCOS.
When the cells become resistant to the action of insulin, the pancreas needs to pump more of this hormone into the blood. People with insulin-resistant PCOS are generally overweight and experience symptoms of brain fog and fatigue.
Post-pill PCOS
This occurs in people when they stop taking oral contraceptive drugs.
Stopping the intake of Ginet, Yasmin, and Yaz is usually responsible for this type of PCOS. You see, when you are no longer taking progesterone-based pills, your ovaries will see a surge of androgens (i.e., male hormones) that lead to acne, excess hair growth, and irregular periods.
Adrenal PCOS
Adrenal PCOS is due to an abnormal stress response that affects 10% of PCOS patients. The hormone DHEA-S is usually elevated alone.
To get diagnosed with this condition, you will most likely need to see an endocrinologist who specializes in hormonal disorders.
Inflammatory PCOS
When chronic inflammation promotes the excess section of testosterone, inflammatory PCOS sets in.
Some signs and symptoms of inflammatory PCOS include:
Headaches
Joint pain
Skin problems (e.g., eczema)
Irritable bowel syndrome
Symptoms of PCOS
As the name implies, PCOS is characterized by a substantial number of cysts that cover the ovaries along with:
High levels of androgens (male hormones)
Irregular menses
These three findings make up the classic triad of PCOS symptoms, which lead to further complications.
For instance, the high levels of testosterone-derivative hormones lead to acne and excessive hair production in females. Additionally, the interrupted menses and cysts cause reversible infertility.
Other symptoms include:
Difficulty getting pregnant
Excessive hair growth on the face, chest, back
Weight gain
Thinning hair
Oily skin or acne
Diagnosis of PCOS
To diagnose PCOS, doctors need to identify at least two of the following symptoms:
High androgen levels
Irregular menstrual cycles
Cysts in the ovaries
Your doctor will also ask about other symptoms, such as acne, body hair, and weight fluctuations.
The next step would be a pelvic exam to evaluate any problems in the reproductive tract. Your doctor will insert their fingers inside the vagina to look for any abnormal growths.
When the physical exam is complete, it is time to test your hormone levels (e.g., cholesterol, insulin, androgens).
Finally, an ultrasound may be used to assess for abnormal follicles and other problems affecting the ovaries and uterus.
This table summarizes key aspects of Polycystic Ovary Syndrome (PCOS):
Aspect
Details
Definition
A hormonal disorder that affects about 10% of women. It causes ovarian cysts, high androgen levels, and irregular periods.
Causes
70-80% of cases are linked to insulin resistance, inflammation, and genetics.
Symptoms
Irregular periods (affects 85% of cases), acne, excess hair growth (70%), weight gain (50%), and infertility.
Diagnosis
Clinical symptoms, hormone tests, and ultrasound (detects ovarian cysts in about 75% of cases).
Treatment
Lifestyle changes (e.g., exercise, diet), medications (e.g., metformin, contraceptives), and skincare.
Complications
Diabetes (50% risk), infertility (40%), and heart disease.
Treatment of PCOS
Patients with PCOS can benefit from lifestyle modifications, including more exercise and healthier dietary choices.
Moreover, drugs such as metformin, oral contraceptives, and clomiphene can also be beneficial.
However, you can still address PCOS-induced acne by taking better care of your skin.
Frequently Asked Questions (FAQs)
How does PCOS affect the pregnant woman and her baby
Pregnant women with PCOS may undergo miscarriage or early loss of pregnancy. According to research, pregnant women with PCOS are three times as likely to miscarry in the early months.
Will removing the ovaries get rid of PCOS?
Yes.
Removing the ovaries means that there is no chance for abnormal cystic growths to occur in the ovaries.
What is the relationship between age and PCOS?
While being close to menopause translates to regular menstrual cycles, it does not necessarily mean that your symptoms will improve. This is because the hormonal imbalances persist despite advanced age.
How does PCOS affect menstruation?
PCOS leads to hormonal imbalances that irregulate your menstrual cycles.
What is the impact of PCOS on pregnancy chances?
PCOS is one of the most common irreversible causes of infertility in women. Due to the irregular menstrual cycle and the defective growth of follicles, the chances of pregnancy are substantially lower.
What you should and should not eat?
If you have PCOS, here is a list of foods that may help with your condition:
Natural, unprocessed foods
High-fiber foods
Fatty fish (e.g., salmon, tuna, sardines, mackerel)
Kale
Spinach
Broccoli
Cauliflower
Dark red fruits (e.g., red grapes, blueberries, blackberries, cherries)
Foods to avoid include:
Refined carbohydrates (e.g., white bread)
Fried foods
Sugary beverages (e.g., sodas, energy drinks)
Processed meats (e.g., hot dogs, sausages)
Solid fats (e.g., margarine, shortening)
Can you use a fertility monitor when you have PCOS?
Using a fertility monitor when you have PCOS will not do you much good. The irregular menstrual cycle and hormonal imbalances make this step futile.
How does PCOS affect breastfeeding?
Women with PCOS tend to have excess estrogen levels in their bloodstream, which interferes with lactation.
To increase your chances of successful breastfeeding, speak with a certified lactation consultant after giving birth.
Takeaway message
PCOS is an extremely prevalent condition that affects millions of women around the world. It is the number one reversible cause of infertility.
We hope that this article managed to introduce PCOS, as well as its common causes, symptoms, and treatments.
Understanding Thyroid Disorders - Symptoms And Treatment Options
Overview
The thyroid is a small gland that’s located at the front of your neck and produces T3 and T4 (e.g., thyroid hormones).
Thyroid hormones control numerous physiological functions, including metabolism, body temperature, and mood fluctuations. However, the production of these hormones may be disrupted.
According to the American Thyroid Association (ATA), approximately 20 million Americans have some form of thyroid disease. Another staggering statistic is that about 12% of the U.S. population will develop a thyroid condition during their lifetime.
For instance, patients with low thyroid hormone levels often complain of experiencing apathy, mood swings, and psychomotor dysfunction. Conversely, when the gland produces excessive amounts of thyroid hormones, the body shifts into hyperthyroidism, which may present with tachycardia (rapid heartbeat), anxiety, weight loss, and restlessness.
In this article, we will discuss the clinical presentation of thyroid disorders, including hyperthyroidism and hypothyroidism. We will also list the available treatment options for these conditions.
Thyroid testing
To comprehensively address thyroid hormone issues, we need sensitive and specific testing of thyroid hormones. Once a diagnosis has been made, your healthcare provider will come up with an appropriate treatment plan that includes pharmacological drugs, diet, and other measures.
A full thyroid panel must test for:
TSH
fT4
fT3
rT3
Anti-TPO antibodies.
Anti-TG antibodies.
SHBG.
Note that thyroid hormone production is linked with several other functions, including inflammation, methylation, nutritional status, toxins in the blood, and the presence of cardiovascular risk factors. So, if your thyroid issues are caused by other underlying conditions, your doctor may need to request more tests.
Sometimes, it may be necessary to check the function of the adrenal glands (e.g., cortisol production). Other tests may also include estrogen, progesterone, testosterone, full blood sugar panel, and food intolerances.
What is hyperthyroidism?
Hyperthyroidism refers to elevated levels of thyroid hormones in the blood. Because these hormones play a role in virtually every cell of the body, you can expect all sorts of signs and symptoms. About 1.2% of the U.S. population (about 1 out of every 100 people) has hyperthyroidism.
The symptoms of hyperthyroidism
Common signs and symptoms of hyperthyroidism include:
Increased appetite
Tachycardia (i.e., fast heartbeat)
Difficulty sleeping
Brittle hair
Restlessness
Distractibility
Weakness
Itching
Hair loss
Nausea and vomiting
The diagnosis of hyperthyroidism
The diagnosis of this condition relies on measuring the levels of thyroid hormones in the blood. When T3 and T4 are elevated, the diagnosis is straightforward.
The treatment of hyperthyroidism
The treatment of hyperthyroidism consists of:
Medication – Antithyroid drugs, such as methimazole, which stop the thyroid from making T3 and T4.
Radioactive iodine – This treatment is given to the vast majority of Americans with hyperthyroidism. It neutralizes the action of the cells that produce large amounts of thyroid hormones.
Surgery – The removal of a section of your thyroid can be an option, especially if you fail to respond to other treatment measures. However, it is left as a last-resort treatment.
What is hypothyroidism?
Hypothyroidism is the exact opposite of hyperthyroidism. In this case, the thyroid gland is not secreting enough hormones, which disrupts the functions of your cells.
Since T3 and T4 provide energy to the body, regulate blood pressure and digestion, and control your metabolism, expect all these functions to get disrupted in case of hypothyroidism.
Most commonly, this condition affects people over the age of 60. However, it could occur at any age, especially when there is an underlying immune disease.
In a 2019 meta-analysis, researchers found that subclinical hypothyroidism is actually linked to depression. In other words, many cases of depression may be caused by asymptomatic hypothyroidism. This is no surprise when you learn that up to 60% of individuals with thyroid disease are unaware of their condition.
Moreover, another link between hypothyroidism and low levels of serotonin was established, which was quickly reversed after the administration of synthetic thyroid hormones.
The symptoms of hypothyroidism
Hypothyroidism affects all organ systems. About 4.6% of the U.S. population (about 5 out of every 100 people) has hypothyroidism (including subclinical cases).
Here are the most common signs and symptoms of hypothyroidism:
Feeling tired all the time
Dry hair and skin
Hypersomnia (i.e., sleeping long hours)
Muscular atrophy
Cold extremities
Mood swings and depression
Bulged eyes
Hoarseness
Constipation
Brittle hair
Decreased libido
Myalgia and arthralgia
Peripheral edema (swelling)
Unexplained weight gain
Carpel Tunnel Syndrome
Irregular menses
Heart palpitations
The diagnosis of hypothyroidism
The diagnosis of hypothyroidism is suspected when a patient presents with the symptoms listed above. To confirm this diagnosis, blood tests of thyroid hormones are necessary.
The treatment of hypothyroidism
The management of hypothyroidism mostly focuses on levothyroxine. The latter is a synthetic T4 hormone that restores normal levels and resolves most symptoms. Some individuals may also benefit from a combination T4/T3 therapy if they remain symptomatic.
It is also vital to address nutritional deficiencies (e.g., iodine, selenium) as they may impede the production of thyroid hormones.
Finally, lifestyle modifications, such as stress management, healthy eating, and regular exercise, can all improve your outcome.
The following table summarizes the major aspects of thyroid disorder:
| Feature | Hypothyroidism | Hyperthyroidism |
|---|---|---|
| Definition | Under-active thyroid gland (insufficient T3 & T4 production). | Overactive thyroid gland (excessive T3 & T4 production). |
| Prevalence (US) | 4.6% of the population. | 1.2% of the population. |
| Common Causes | Autoimmune (Hashimoto’s thyroiditis). Iodine deficiency. Post-thyroid surgery or radioactive iodine treatment. Certain medications. | Autoimmune (Graves’ disease). Thyroid nodules. Excessive iodine intake. Thyroiditis (inflammation). |
| Typical Symptoms | Fatigue and weight gain. Cold intolerance. Dry skin/hair. Constipation. Depression and mood swings. Bradycardia (slow heart rate). | Weight loss and increased appetite. Heat intolerance. Palpitations/tachycardia. Anxiety and restlessness. Insomnia. Brittle hair/hair loss. Tremors. |
| Diagnosis | Elevated TSH, low T4/T3. Check for anti-TPO and anti-Tg antibodies. | Low TSH and high T3/T4. Check for TRAb (TSI in Graves’ disease). Thyroid uptake scan. |
| Treatment | Synthetic T4 (Levothyroxine). Possible combination T4/T3. Lifestyle and nutritional support. | Antithyroid drugs (e.g., methimazole). Radioactive iodine therapy. Surgery (last resort). |